Teaching goals and learning objectives
EAHP Academy Seminar 2015
An ACPE application based activity
ACPE Universal Activity Number (UAN): 0475-0000-15-032-L04-P/CEUs: 1.4
Academy Seminars on Medication Reconciliation, Medication Review and Medicines Optimisation
About medicines reconciliation (also referred to as medicines optimisation)
In 2006, the World Health Organization (WHO) began the High 5s programme. Medicines reconciliation was a target and due to the complexity and resource requirement, their focus was on patients 65 years of age and older, who were admitted to an inpatient ward from the emergency department. The Institute of Healthcare Improvement (IHI) also set medicines reconciliation as one of its work streams in their ‘Saving Lives campaign’. In the UK from 2004 to 2008, IHI together with the Health Foundation (HF) launched the Safer Patients Initiative. They also set a target on medicines reconciliation and acknowledged that this could be a slow process due to the complexity.
Medication Reconciliation is defined by the US Joint Commission as “the process of comparing the medications a patient is taking (and should be taking) with newly ordered medications”. It is designed to ensure that a patient’s medication history is identified and addressed in the hospitalization process. When organisations do not consistently and reliably reconcile patient medications across the continuum of care, medication errors and adverse drug events occur. About 20% of all adverse drug events have been attributed to poor communication at the transition and interfaces of care.
The need
Medicines reconciliation has been an emerging topic in EAHP Congresses for a couple of years. Although there is no objection to the importance, no uniformity could be seen in the methodologies used in submitted abstracts. This lacking part of quality management and pharmaceutical support is one of the declared targets to explore in this Academy seminar. The topic is too important to let grow a multitude of not harmonised methods and develop an auto-dynamic reconciliation practice in European hospitals.
Evidence is needed to demonstrate that pharmacists do best medicines reconciliations. The reality of the staffing situation must be evaluated, if hospital pharmacy should warrant an added value of its performance and capabilities, performances by technicians and nurses, while being supervised by a pharmacist, must be assessed. There must be clarity in the responsibility for the SOPs, training and the more complex medicines reconciliations. For all those who are new in medicines reconciliation, practicalities should be harmonised all over Europe: How to set up the service? How to staff? When to do medicines reconciliation (only on admission if resources are short?)? How to get the necessary logistics changes done in the hospital medication list? How to document medicines reconciliation in the case notes? What "added extras" can medicines reconciliation offer?
Lots of interfaces to other disciplines are needed to effectively and successfully reconcile medications. Pharmacy contribution to multidisciplinary task forces is likely to have added values, according to studies, which focus mainly on patient admission. This should be expanded as a continuing reconciliation and support until the patient's discharge, thus from Medicines Reconciliation to Medicines Optimisation and Medicines Review.
Reconciliation is at the interface of procurement, clinical pharmacy and patient safety. It is also addressed in the European Statements of Hospital Pharmacy. According to statement 2.7, hospital pharmacists should be involved in the development of policies regarding the use of medicines brought into the hospital by patients. In addition, according to statement 4.4, all the medicines used by patients should be entered on the patient’s medical record and reconciled by the hospital pharmacist on admission. Hospital pharmacists should assess the appropriateness of all patients’ medicines, including herbal and dietary supplements. In line with statement 5.6, hospital pharmacists should ensure that high-risk medicines are identified and implement appropriate procedures in procurement, prescribing, preparing, dispensing, administration and monitoring processes to minimise risk. As a result, the hospital pharmacy contribution to medications reconciliation consists of:
- Policy and procedure development
- Implementation and performance improvement
- Training and competency assurance
- Information systems development
- Advocacy
In addition to these European Statements of Hospital Pharmacy, the need is also arising from hospital pharmacy practice, since the topic "medication reconciliation" has been proposed in the Cyber Café Survey at the EAHP Congress 2014 in Barcelona and from the EAHP Scientific Committee.
Links to the European Statements of Hospital pharmacy
The needs, the contents and the findings of this Academy seminar will cover the following statements of the European Statements on Hospital Pharmacy:
- Section 4: Clinical Pharmacy Services (Statements 4.1 – 4.8)
- Section 5: Patient Safety and Quality Assurance (Statements 5.1 – 5.11)
Teaching Goals and Learning Objectives of the Academy Camp and the Workshops
Teaching goals:
-
To teach current medicines reconciliation methodologies and research findings
-
To profile the target groups of patients needing reconciliation
-
To trail the reconciliation process and break it down into a consistent workflow of single steps which starts at the anamnesis and ends with the complete medication log in the electronic patient documentation at dischargeLearning Objectives
-
To identify standardisation and harmonisation options
-
To draft a SOP of European Medicines Reconciliation, guidelines and/or recommendations (as a take home document)
Target group of the seminar
The target group comprises clinically oriented hospital pharmacists at the interface of R&D and practice, mainly heads and/or deputy heads of pharmacy, particularly those from the new EU countries and new members of EAHP.
Didactic tools
There will be introductory lectures about the most relevant subchapters of medicines reconciliation right before the workshops will start. The messages delivered during the introductory lectures will be applied and systematised in breakout sessions and plenary discussions. Breakout sessions will serve to develop a catalogue and classification, statements, standards and policy drafts, checklists and guidelines or recommendations. Communication methods used in medicines reconciliation will be demonstrated as well as trained and peer-reviewed in plenary. Groups are selected according to country-similarity. Flow-charts and mind maps will be designed using X-mind® freely available on the web. Laptops, beamers (and flipcharts), handycam / video equipment will be used as didactic and e-learning tools.
Evaluation of the seminar – Dissemination of take home messages
The EAHP has partially delegated evaluations of the Academy Camps to the National Associations. In general, presentations and workshop results will be reported back to the associations' members as presentations in the course of General Assemblies or at separate symposia. To facilitate reporting and multiplying knowledge in the national associations, delegates will receive summary slides from the presentations and documents from the workshops. National Assemblies confirm the completion of multiplication to EAHP.
Contents, Teaching Goals, and Learning Objectives of the lectures
"Systematic Approach and Challenges of Medicines Reconciliation"
Dr Fatma Karapinar, Epidemiologist, Sint Lucas Andreas Ziekenhuis, Amsterdam, the Netherlands
Abstract
In daily practice, medication reconciliation is too often seen as a process to obtain a medication list without an evaluation regarding what's on the list. It involves a three-step process:
- Verification (collecting an accurate medication history)
- Clarification (ensuring that the medications and doses are appropriate)
- Reconciliation (documenting every single change and making sure it "squares" with all the other medication information).
In daily practice generally only the verification step is performed. Any new medication added is not evaluated. Therefore, there are still patients who are discharged with hypnotics, laxatives, proton pump inhibitors etc. which do not have an indication anymore at discharge. Medication reconciliation at hospital discharge focuses too often on admission, but the length of stay decreases in hospitals. For continuity of pharmaceutical care, thus the focus needs to be aimed at discharge and on collaboration with primary care as well. The process at discharge is far more complex that it is at admission. The consequences can also be major (e.g. a physician that forgets to re-start anticoagulation after a surgery). Also there are multiple problems post-discharge. A recent study showed that patients have DRPs within 72 hours post-discharge, despite medication reconciliation at hospital discharge. So hospital pharmacists need to think broader than the walls of their hospitals.
Further challenges of medication reconciliation comprise:
- The role of the patient and his carer. How can we involve patients in performing the verification step themselves? This could lead to additional time for the pharmacist to evaluate a list instead of collecting one.
- The role of IT. We lack manpower to perform medication reconciliation for every (high-risk) patient. How can we use IT smarter? There is quite some literature on this topic, and we are trying to conduct a study ourselves.
Teaching goals
In this section, the presenter will:
- Define Medication Reconciliation (according to the IHI definition ("Medication reconciliation is the process of creating the most accurate list possible of all medications a patient is taking ... with the goal of providing correct medications to the..."))
- Compare the NL way to alternative approaches of medicines reconciliation
- Address the 3 main steps of medication reconciliation in order to promote to a true medicines optimisation
Learning objectives
At the end of this session, participants will be able:
- To reproduce recommendations according to quasi standards in use
- To report back the medicines reconciliation policies to the national association
"Medicines Reconciliation on Admission"
Mrs Jane Smith, Principal pharmacist, Development & Governance, NBT Medication Safety Officer (MSO), North Bristol NHS Trust, Bristol, UK
Abstract
"The aim of medicines reconciliation on hospital admission is to ensure that medicines prescribed on admission correspond to those that the patient was taking before admission. Establishing correct medications details may involve discussion with the patient and/or carers and the use of records from primary care. "
In some countries this process also includes a review of the Patients Own Drugs (PODs). Medicines Reconciliation should occur on admission, on transfer and on discharge. This workshop will focus on medicines reconciliation on admission because this is a complex area as information from primary care and patients and/or carers is not always easy to obtain. Furthermore, patients do not always use their medicines the way their health professionals think.
Our experiences of achieving medicines reconciliation have involved the use of quality improvement tools (for example the "Safer Patients Initiative" involving the use of the Model for Improvement and PDSA (plan, do study, act) cycles). Typically, this can begin on one ward, followed by ongoing tests of change, measurement and displaying run charts to spread and embed medicines reconciliation.
Pharmacists and Pharmacy Technicians, thanks to their expertise and training, have an opportunity to help lower the burden of medication discrepancies through their input in Medicines Reconciliation.
Teaching goals
In this section, the presenter will:
- Present the principles and strategies to spread and measure the improvements in Medication Reconciliation
- Describe the interdisciplinarity and shared responsibility for the patient care
- Present why Medication Reconciliation on admission is important in health care settings (showing the evidence, benefits, cost savings)
- Demonstrate how to implement Medication Reconciliation on admission in a hospital setting; how to measure the process, demonstrate improvements and engage collaboration with the multidisciplinary team
- Present the key factors to gain the support to spread and embed in an organisation
Learning objectives
At the end of this session, participants will be able:
- To understand and describe the importance of the Medication Reconciliation process
- To recognise the pharmacist's (and technician's) role in this process
- To describe the importance of Medication Reconciliation process
- To present the principles and strategies to spread and measure the improvements in Medication Reconciliation beyond pilot unit
- To recognise the pharmacist and pharmacy technician's role in this process
"Lessons Learnt for Successful Implementation of Medicines Reconciliation"
Dr André Rieutord, Hôpital Antoine Béclère/ Service Pharmacie, Clamart, France
Abstract
The pharmacy of Antoine Béclère Hospital experienced 6 years of practice in different clinical settings. We consider that starting Medication reconciliation is very exciting but one always has to consider the sustainability of the process when implemented. Through our medication reconciliation story board, we will highlight problems encountered after implementation. The pharmacist as any project manager must define a strategy, identify the barriers (human factors, quality, training, technology...) and propose collaborative solutions according to the given context. Business process improvement using "Kaizen" approach will be considered and illustrated with concrete examples.
Teaching goals
In this section, the presenter will
- Discuss implementation strategies for pharmacy involvement in medication reconciliation
- Highlight methods to overcome barriers encountered during implementation
- Identify metrics and quality assessment tools and techniques which facilitate ongoing process improvement
Learning objectives
At the end of this session, participants will be able:
-
To describe all steps of medication reconciliation process
-
To identify the steps missing in their own institutions and to complete accordingly
-
To establish a real and effective collaborative approach for the entire process
-
To identify barriers in the process
-
To develop a bottom up approach to solve problems
"Clinical Implementation – Integrated Medicines Management with focus on the discharge process"
Prof Dr Tommy Eriksson, Lund University, Lund, Sweden
Abstract
The Lund Integrated Medicines Management (LIMM) -model with pharmacists as the driver has been developed, researched and implemented over 15 years. Now the model has been fully implemented in the eight hospitals of the County of Skåne (south of Sweden). The Med Rec process is the base for the team activities where the pharmacist and the physician has different but complementary roles. Clinical-, economic- and humanistic outcomes will be presented based on patient focus and safety, quality, systematic activities, educational aspects and payment for performance. There will also be a focus on discharge Med Rec. What information do the patient and the next level of care need and how can it be presented and communicated.
Teaching goals
In this section, the presenter will:
- Present the LIMM model
- Demonstrate crucial aspects for the implementation
- Discuss the pharmacist's role for development, education and implementation
- Discuss responsibilities, aims and quality in the discharge Med Rec process based on the patient's perspective
Learning objectives
At the end of this session, participants will be able:
- To overlook successes and pitfalls of integrated medicines management
- To MUST-do in the discharge Med Rec process
- Use patient safety and quality aspects to plan for the best discharge Med Rec process
"The Impact of Medicines Reconciliation and Structured Patient Interviews on Error Incidence and Severity"
Dr Ulrika Gillespie, Uppsala University Hospital, Uppsala, Sweden
Abstract
Many studies have been performed worldwide to try to determine the magnitude and consequences of medication errors that occur when patients are being transferred between caregivers. Again, many studies have looked into the effects of different strategies aiming at minimizing the risk of errors. In this session the focus is on the effects of medication reconciliation performed by pharmacists and on trying to summarize the current evidence base.
Medication reconciliation is sometimes carried out without including a patient interview (mostly due to time constraints). There is debate however, to whether it is even possible to claim that a medication reconciliation has been performed if the patient has not been involved, confirming the actual use of the drugs on the reconciled list. In this session the importance of the additional information gained from the interview will be demonstrated and discussed along with a description of key items to include in the interview.
Teaching goals
In this section, the presenter and workshop coach will
- Present the current evidence base for effects and impacts medicines reconciliation on error prevalence and on clinical- and health economic outcomes
- Demonstrate qualitative and quantitative effects including a structured of patient interview in the medication reconciliation process
- List determinant and mandatory items of the structured patient interview
Learning objectives
At the end of this session, participants will be able
- To summarize the current evidence base for effects of medication reconciliation
- To describe the importance of patient interviews in the medication reconciliation process
- To identify MUST-asks of patient interviews
"Structured Patient Interviewing and Physician Communication to resolve Med Rec Problems – Demo of Quality and Educational Aspects"
Prof Dr Tommy Eriksson, Lund University, Malmö, Sweden
Dr Ulrika Gillespie, Division of Pharmacokinetics and Drug Therapy, Department of Pharmaceutical Biosciences, Uppsala University and Uppsala University Hospital, Uppsala, Sweden
Abstract
The oral structured clinical examination by the hospital pharmacist comprises the two steps as follows:
- Patient interview, i.e. identifying incorrect medications in the medication list
- Physician discussion, i.e. implementing the correct medication list
Teaching goals
In this section, the presenter sand workshop coaches will:
- Describe and demonstrate a method for training pharmacists to identify and resolve admission Med Rec problems
Learning objectives
At the end of this session, participants will be able:
- To understand the importance of systematic training sessions to improve patient care
- To describe the demonstrated model
- To implement a (the?) model in their own environment
- To communicate with educational and professional bodies in order to implement a (the?) national systematic training module
Contents, Teaching Goals, and Learning Objectives of the workshops
Plenary Workshop: Simulation and peer-reviewed video sequences
Abstract
The afternoon presentations and the afternoon workshop will consist of a demonstration of the structured interview technique followed by the integration of the delegates into a discussion and evaluation of the demo interviewing, as well as role plays after the coffee break. In order to train typical communication scenarios between pharmacist and patient, role plays of the structured patient interview will give the delegates a representative impression of best practice and of using standardised procedures to train pharmacists in medication reconciliation. The role plays will be registered and video sequences discussed in plenum.
Teaching goals
In this section, the workshop coaches will:
- Supervise role plays performed by a selection of the delegates
- Animate the critical peer-review and assessment of the role play records by the delegates and demonstrate how role plays can be used in the form of an OSCE (Objective Structured Clinical Examination) to train pharmacists
Learning objectives
At the end of this session, participants will be able:
- To assess the most promising interview techniques
- To identify critical elements of patient interviews
- To introduce the OSCE model for training pharmacists in their own setting
Interactive Podium-Discussion on further aspects and seamless medicines reconciliation
Abstract
In order to evaluate added values for the therapist (and their interest in the clinical outcome), for taxpayers (and their interest in the financial outcome), and for patients (and their interest in extended QALYs), an interactive podium discussion on further elements and the interfaces at patient admission and discharge is held. Current approaches of medicines reconciliation concentrate on admission and on discharge. Supervision of further aspects of pharmacotherapy along the entire hospital stay may contribute to better outcomes as well. The pharmacist's contribution to medicines reconciliation, optimisation and review may comprise laboratory data (point of care testing), or the phenotype of the patient.
The interactive podium discussion will be a moderated discussion and will include presumably items such as "the Gold Standard - pharmacy and/or patient's records", qualification aspects, training aspects, inappropriate pharmacotherapy, "beyond simple lists - drug related problems to be reconciled".
Elements of this discussion will be used in the following parallel workshop on systematisation.
Teaching goals
In this section, the workshop coaches will:
- Expand procedures from admission along the time line up to discharge of the patient including their documentation
- Discuss how additional information from laboratory data (point of care testing), phenotype, personal situation of the patient after discharge will impact medicines optimisation
- Animate the delegates' participation in harmonisation approaches by setting statements on which interactive contributions from the delegates will be given
Learning objectives
At the end of this session, participants will be able:
- To overview essential further information needed for integrated medicines optimisation
- To overview essential further information needed for medicines optimisation
- To define targets at the patient's discharge
Parallel workshops on systematisation, cataloguing, and harmonisation (World Café Style)
Abstract
Inputs from the introductory presentations arising from research and practice now have to be recombined to a comprehensive overview of the relevant elements of medicines reconciliation. Experiences of the delegates and regional or national approaches have to be brought together. The catalogue of the elements of medicines reconciliation will be broken down into a consistent workflow of single steps, which starts at the anamnesis and ends with the complete medication log in the electronic patient documentation at discharge.
The 4 parallel workshops will develop the following take home deliverables:
- The EAHP Medicines Reconciliation SOP (starting from the WHO High 5s programme)
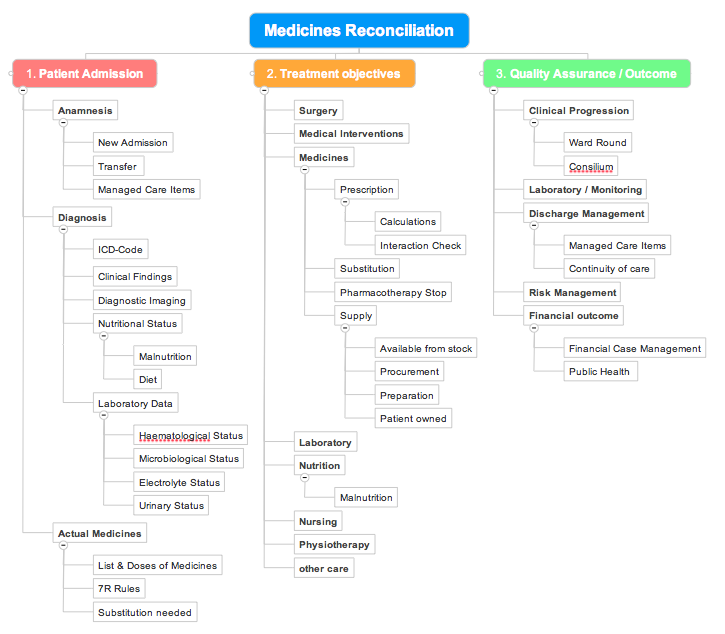
- The Scope: Systematic and comprehensive mindmap of the elements of Medicines Reconciliation
- The Process of Medicines Reconciliation: Flow chart and Procedures
- Medicines Reconciliation on Admission
- Integrated Medicines Management on the entire hospital stay
- Medicines Reconciliation on Discharge
- Draft EAHP Reconciliation Statements (starting from the EAHP statements of Hospital Pharmacy)
Teaching goals
In this section, the workshop coaches will:
- Animate brainstorming
- Supervise the drafting of EAHP Medicines Reconciliation SOP
- Guide the design of mind-maps (using Xmind® or Mindjet Mind-Manager®), which define the Scope of Medicines Reconciliation
- Guide the design of the process workflow chart
- Supervise the drafting of EAHP Medicines Reconciliation SOP
Learning objectives
At the end of the workshops, participants will be able:
- To overlook elements and procedures of medicines reconciliation arising from the international approach in this workshop
- To understand the European Medicines Reconciliation SOP
- To animate the implementation of standardised Medicines Reconciliation in the hospital of the own employer and in further hospitals of the home country
References
- University Hospital of South Manchester NHS Foundation Trust - Medicines Reconciliation. V 1, 2009.
- The Newcastle upon Tyne Hospitals NHS Foundation Trust – Medicines Reconciliation Policy and Procedure
- National Institute for Clinical Effectiveness (NICE) and the National Patient Safety Agency (NPSA). Technical patient safety solutions for medicines reconciliation on admission of adults to hospital. Issue date: December 2007. Alert reference: NICE/NPSA/2007/PSG001. http://www.nice.org.uk/guidance/psg001/evidence/full-guidance-pdf2. Retrieved on 4 January 2015.
- ASHP. ASHP Statements on the pharmacist's role in medication reconciliation. Am J Health Syst Pharm 2013;70(5):453-6. doi: 10.2146/sp120009.
- http://www.jointcommission.org. retrieved on 4 January 2015.
- N.N. Improving medicines reconciliation on admission. Hospital Pharmacy Europe. 2014;74. http://www.hospitalpharmacyeurope.com/featured-articles/improving-medici.... Retrieved on 4 January 2015.
- Medicines interchange guide. http://gruposdetrabajo.sefh.es/genesis/index.php?option=com_content&view...





